
Vitamin D is often treated like a simple daily add-on. It is tied to bone health, calcium balance, muscle function, and immune support, so many adults take it without thinking of it as something that can interact with prescription drugs.
But vitamin D does not act alone in the body. It shares absorption pathways, affects calcium levels, and can overlap with liver enzymes that also handle medications. That is why a supplement routine can become more complicated for people taking long-term medicines for cholesterol, blood pressure, heart rhythm, inflammation, or digestion.
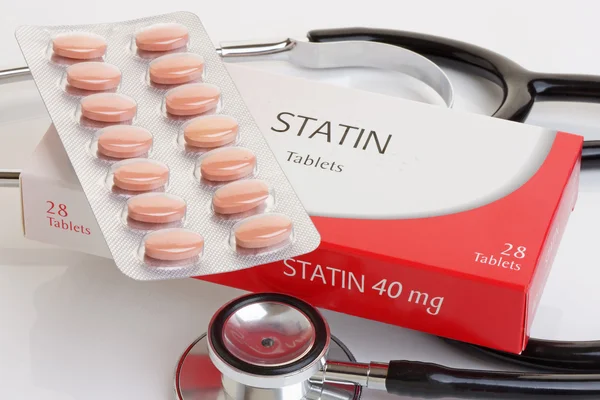
1. Statins
Some statins and vitamin D appear to overlap in ways that are still being studied. The biggest concern involves statins that rely on the CYP3A4 enzyme pathway, including atorvastatin, lovastatin, and simvastatin. A systematic review found that atorvastatin may raise vitamin D levels, while vitamin D supplementation may lower atorvastatin concentrations.
The research is not strong enough to support broad rules for every patient, but it does show that the pairing is not always neutral. Newer evidence also undercuts one popular belief: in a large randomized trial, vitamin D did not prevent statin-associated muscle symptoms, even in participants with lower vitamin D levels.
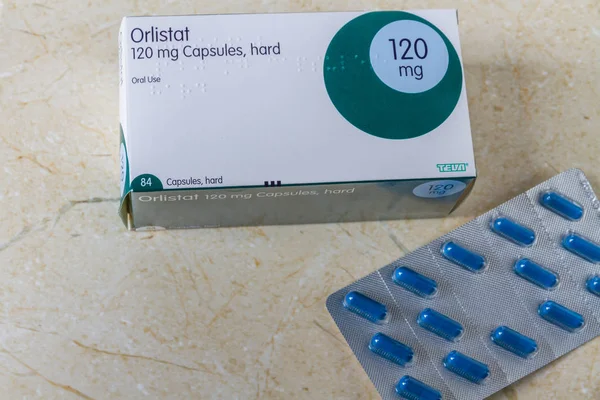
2. Orlistat
Orlistat can interfere with vitamin D before the vitamin ever reaches the bloodstream. Because vitamin D is fat-soluble, anything that blocks fat absorption can also reduce vitamin D absorption. That is why this combination matters over time.
In clinical studies reviewed in the literature, people taking orlistat showed drops in vitamin D levels, although lower-fat eating patterns may have contributed as well. The practical issue remains the same: people using orlistat may need monitoring for vitamin D status and may need to separate dosing by several hours.
3. Thiazide Diuretics
Thiazide diuretics such as hydrochlorothiazide deserve extra attention because they reduce calcium loss in urine, while vitamin D increases calcium absorption from the gut. Together, they can push calcium upward. This interaction is most concerning in older adults and in people with kidney disease, hyperparathyroidism, or high calcium intake from other supplements.
A trial in Black adults found that vitamin D3 up to 4000 IU daily with hydrochlorothiazide raised calcium slightly, but hypercalcemia was uncommon. Even so, case reports in older patients show the risk becomes more meaningful when vitamin D is combined with thiazides and substantial calcium intake.

4. Corticosteroids
Prednisone, dexamethasone, and related corticosteroids are well known for their long-term effects on bone. Their relationship with vitamin D is less straightforward than many supplement labels suggest. Research reviewed in human studies found mixed results on whether steroids significantly lower circulating vitamin D itself.
What is clearer is that corticosteroids can impair calcium handling and contribute to bone loss over time. For adults on chronic steroid treatment, vitamin D may still be relevant, but the issue is less about a simple drug clash and more about ongoing monitoring of bone and mineral health.

5. Bile Acid Sequestrants
Cholestyramine, colestipol, and colesevelam can create a problem in the intestine. These drugs bind bile acids, and bile acids help the body absorb fat-soluble vitamins such as vitamin D. The research has not been perfectly consistent, but the mechanism is clear enough to make timing important. Taking vitamin D well before these medicines can help reduce the chance that the supplement gets trapped in the gut instead of absorbed.
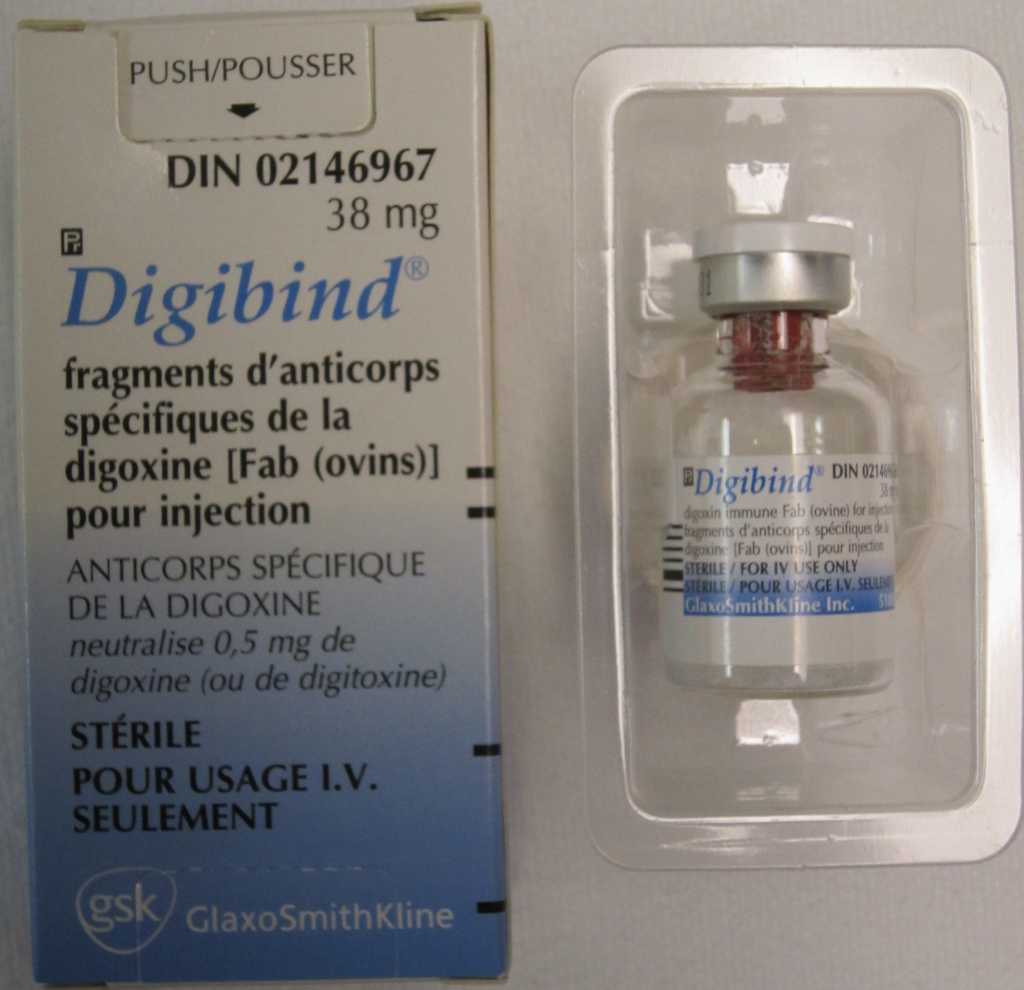
6. Digoxin
Digoxin has a narrow safety margin, which makes calcium changes more important. When vitamin D intake becomes excessive, calcium can rise, and that can make digoxin-related rhythm problems more dangerous. This is not mainly a concern with ordinary vitamin D use. It becomes more serious when high doses are added on top of calcium supplements or other medicines that also influence calcium balance. For patients on digoxin, the risk is less about vitamin D itself than about letting calcium drift too high without noticing.

7. Diltiazem
Diltiazem is another medicine where calcium balance matters. Since vitamin D increases calcium absorption, very high supplement use can complicate management in people already taking drugs for blood pressure or heart rhythm. The evidence here is more limited than it is for thiazides or digoxin, but the overlap is still clinically relevant. Symptoms linked to elevated calcium can include fatigue, muscle weakness, thirst, confusion, nausea, and frequent urination.

8. Mineral Oil
Mineral oil may seem harmless because it is sold over the counter, but it can interfere with absorption of fat-soluble vitamins. That includes vitamin D. For short-term use, the effect is usually mild. The issue becomes more noticeable when mineral oil is used repeatedly or taken too close to vitamin D. Spacing the two apart can help limit the absorption problem.
9. Calcium and Magnesium Supplements
These are not prescription drugs, but they are among the most common add-ons to vitamin D. That makes them one of the most important combinations to review. Vitamin D helps the body absorb calcium, which is useful when intake is appropriate. But piling high-dose calcium on top of vitamin D, especially with a thiazide diuretic in the mix, can increase the chance of hypercalcemia. Magnesium is different, yet timing still matters because large mineral doses can compete in the gut and complicate a supplement schedule that already includes vitamin D. In practice, the combination is often less about avoiding all overlap and more about avoiding excess.
The larger lesson is simple: vitamin D is a biologically active supplement, not a neutral extra. It can change absorption, shift calcium levels, and overlap with drug metabolism in ways that matter most for people taking chronic medications. For adults using vitamin D regularly, especially alongside heart, cholesterol, blood pressure, or steroid medicines, the safest approach is to review the full medication and supplement list together instead of treating each pill separately.

