
Here’s a surprise: losing your sense of smell can foretell your chances of dying within five years more reliably than most chronic illnesses. That’s no ghostly superstition; it’s supported by rigorous science. Scientists have discovered that declining olfactory ability isn’t merely about smelling the fresh coffee potentially, it can signal deeper health problems.

For years, the underdog of the senses was smell, routinely written off as inferior to sight or hearing. But new evidence is turning that on its head, revealing that the nose is a robust pre-crime detector for vulnerability, dementia, and even death. And in contrast to most medical screens, a sniff test is rapid, painless, and surprisingly informative.
This list explores the intriguing science of smell, why it is more important than most individuals appreciate, and how it may be a revolutionary tool for anticipating and safeguarding long-term health.

1. Smell Loss Strongly Predicts Mortality
Landmark research in PLOS ONE discovered that older people with total loss of smell (anosmia) were more than three times more likely to die within five years than those with typical olfaction-even after controlling for age, gender, education, and serious disease. Indeed, anosmia was a better predictor of mortality than most chronic diseases, second only to advanced liver damage. The scientists tested people between 57 and 85 years old for their capacity to detect five common odors rose, peppermint, leather, orange, and fish and monitored their survival for several years. The findings indicated a definite dose-response relationship: the poorer the smell function, the greater the risk of mortality.
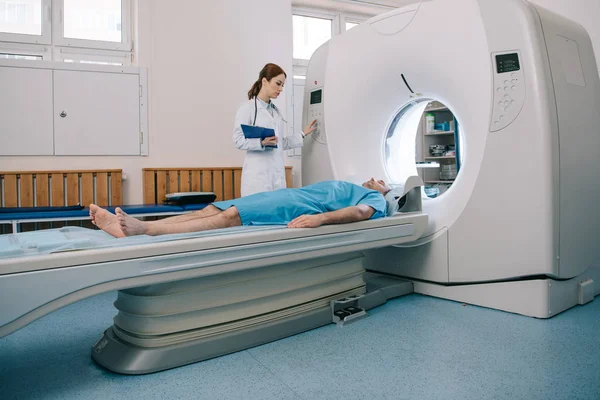
2. Even Mild Decline in Smell Is Significant
Total smell loss is not the only worry. The same study found that even mild impairment of smell (hyposmia) dramatically elevated the risk of death. Every extra misstep in detecting odors was associated with an observable increase in mortality risk. That is, slight alterations such as difficulty sensing certain fragrances can be a early warning signal for health deterioration. Crucially, these impacts remained after adjusting for smoking, alcohol consumption, mental illness, and frailty, indicating smell tests might pick up on dangers which other tests fail to detect.

3. A Window Into Frailty
Smell loss doesn’t only forecast death it’s also associated with frailty, a syndrome characterized by weakness, weight loss, and inactivity. Johns Hopkins scientists discovered that both deficient smell identification and lower sensitivity were associated with greater frailty scores in older people. As Dr. Nicholas Rowan described, “it’s not necessarily your aging brain that is doing this work here, but it could also be something peripheral, such as something at the level of your nose that can anticipate our future frailty and demise.” Low olfactory function can cause malnutrition, safety risks, and social isolation, which all promote frailty.

4. An Evolutionary Survival Tool
From sensing rotten food to smelling fire or gas leaks, smell has ever been a survival tool. Anthropologist Kara C. Hoover points out that human beings evolved to employ smell in searching for healthy food, staying away from poisons, and even choosing mates. Environmental pollution and city life, however, are numbing this prehistoric sense, generating what she refers to as “sensory inequities.” Individuals who live in areas with air pollution tend to have low smell, maybe missing important environmental signals to keep them healthy.
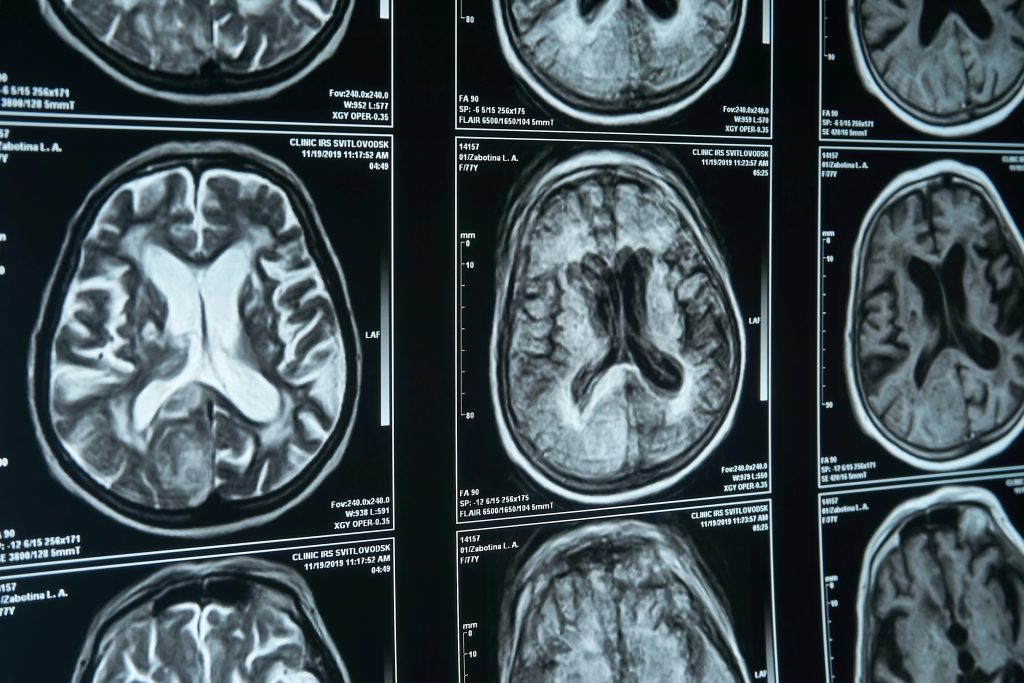
5. Olfactory Loss as a Neurological Indicator
Olfactory loss may be one of the first signs of neurodegenerative diseases such as Alzheimer’s and Parkinson’s sometimes surfacing years before memory failure or tremors. Post-mortem examinations have also identified that the brain transformations responsible for dementia usually start in the olfactory system. According to Dr. Zara Patel of Stanford Medicine, sudden, inexplicable smell loss should never be downplayed as normal aging. Future generations will likely see smell testing as standard as mammograms for detecting disease early.

6. The Emotional and Social Toll
Beyond physical health, losing the ability to smell can be devastating emotionally. Patel’s patients often describe life without scent as “going gray.” It can strip away the joy of eating, disconnect people from cherished memories, and trigger depression affecting up to 76% of those with smell loss. Social rituals built around food and drink become isolating, leading many to withdraw from friends and family. Safety issues also increase, as people won’t notice smoke, gas leaks, or contaminated food.
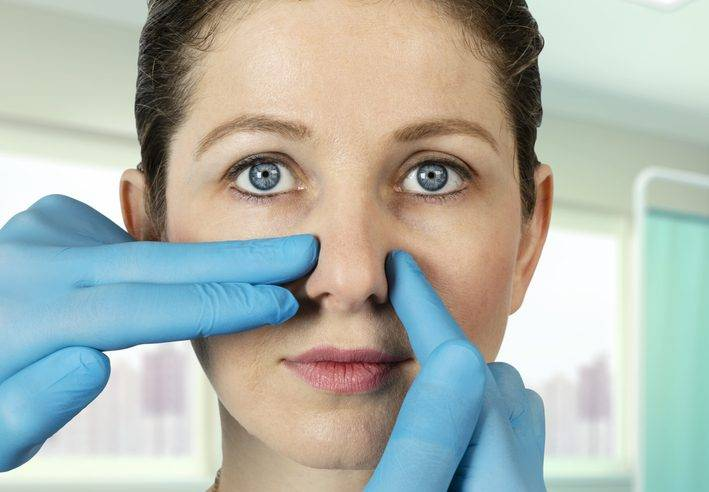
7. Smell Testing and Treatment: New Frontiers
Existing smell tests, such as the University of Pennsylvania Smell Identification Test, are helpful but subjective. Patel is creating a handheld device that directly measures the electrical activity of olfactory neurons, providing an objective method for diagnosing smell loss and perhaps identifying its source. On the treatment end, she’s leading the way in injecting platelet-rich plasma (PRP) into the olfactory epithelium to stimulate growth of destroyed neurons. In initial trials, 57% of patients showed notable improvement providing promise for those who’d lost their sense of smell permanently.

The nose, it happens, is not just a pipe for smells it’s a sensitive health sensor that can detect underlying dangers weeks or months before other signs show up. As investigations continue, smell testing might become an integral part of preventive medicine, enabling frailty, mental decline, and serious disease to be detected early. In the meantime, tuning in to changes in the sense of smell isn’t merely about enjoying the pleasures of life it might just prove to be a lifesaver.

