
When a person is nearing the end of life, the body often changes in ways that can look frightening from the bedside. Families may see less eating, unusual breathing, long stretches of sleep, or periods of restlessness and assume the person is in distress.
Hospice and palliative care guidance describes many of these shifts as common parts of the body’s natural slowing down. That does not mean every symptom should be ignored, but it does mean that appearance and suffering are not always the same thing.

1. Sleeping most of the time
A person who is close to death often becomes much less alert, sleeps for long periods, and may be difficult to wake. Families sometimes read this as giving up or as a sign that the person is uncomfortable and withdrawing because of pain. In many cases, it reflects the body conserving energy as physical systems slow down. Communication and activity levels decrease as death approaches, and many people eventually become unresponsive. Even then, hearing may remain for longer than other senses, which is why calm voices and gentle touch continue to matter.

2. Eating and drinking very little
One of the hardest changes for families to witness is a fading interest in food and fluids. Loved ones often feel that offering nourishment is basic care, so refusal can look alarming or even cruel. Yet in the last days of life, reduced intake is usually a normal part of the process rather than proof of suffering. Hospice organizations consistently advise families not to force food or drink when swallowing becomes difficult. Pushing intake can increase coughing, choking, and discomfort. Comfort care usually shifts toward moistening the mouth, using lip balm, and offering small sips or ice only if the person wants them.
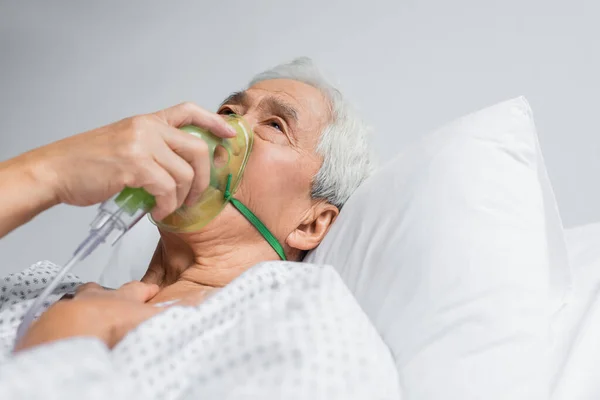
3. Noisy, rattling breathing
This is one of the most upsetting sounds for families. A wet, gurgling noise may develop when a person can no longer swallow or clear secretions well, creating what is commonly called the death rattle. The sound is distressing to hear, but bedside guidance for end-of-life care notes that it does not usually mean pain. Research involving bereaved relatives found that the sound itself can be highly stressful, especially when families worry the person is choking or when they do not know how long it will last. That distinction matters: the family’s distress is real, but it does not automatically mean the patient is suffering in the same way.

4. Irregular breathing with pauses
Breathing near the end of life often stops following a normal rhythm. There may be shallow breaths, faster breaths, and pauses that seem unbearably long to anyone watching. These episodes can make families think the person is gasping in fear or fighting for air. One common pattern is Cheyne-Stokes breathing, in which several breaths are followed by a period of no breathing. Hospice sources describe this as a frequent end-of-life change that may signal death is near. It can be dramatic to witness, but it is generally understood as part of the body’s final physiological changes rather than a clear sign of torment.

5. Cool, mottled, or bluish skin
Hands, feet, knees, and other areas may become cool, pale, gray, or blotchy as circulation shifts away from the skin. Families may fear this means the person feels intensely cold or that something sudden has gone terribly wrong. In most cases, this change reflects decreased circulation as the body shuts down. A soft blanket may help if the person seems chilly, but heating pads are usually discouraged because fragile skin can burn easily. The appearance may be startling, yet it is commonly described as an expected physical sign rather than evidence of pain.
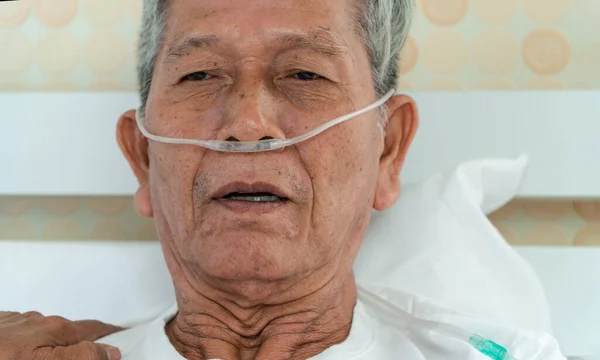
6. Confusion, visions, or talking to people who are not there
Near death, some people become disoriented, misinterpret sounds, or speak about seeing deceased relatives, spiritual figures, or travel preparations. Families may assume this means panic, psychiatric crisis, or medication toxicity. Sometimes these experiences are troubling, but they are also recognized as common sensory changes in the dying process.

Hospice education materials describe illusions, hallucinations, and near-death awareness as changes that may come and go, often becoming more noticeable at night. What matters most is whether the person appears frightened or calm. When the experience seems peaceful, correction is usually less helpful than reassurance.

7. Restlessness or pulling at the sheets
Terminal restlessness can look like severe suffering because the person may fidget, pick at clothing, pull at bedding, or seem unable to settle. Families often interpret every movement as uncontrolled pain. Sometimes discomfort is involved, which is why clinicians pay attention to grimacing, moaning, or resistance to movement. But restlessness can also arise from the metabolic and neurological changes of active dying. According to hospice guidance, these signs aren’t medical emergencies in the usual sense, though they do deserve prompt assessment for comfort needs.

Families at the bedside often judge suffering by what looks or sounds unbearable to witness. End-of-life care literature makes a quieter point: some of the most unsettling signs are part of the body’s normal shutdown, while true discomfort may show up in subtler ways. The most useful response is not to assume, but to observe. A calm face, relaxed body, and peaceful stillness can tell a different story than the sound of breathing or the look of the skin. When uncertainty remains, hospice or palliative care clinicians are the ones trained to tell the difference.

