
The last hours of life often leave families trying to help in every way they know. That instinct is loving, but at the bedside, some of the most common actions can add strain instead of comfort.
Hospice and palliative care guidance repeatedly describes a different approach: less forcing, less correcting, less panic, and more calm presence. In the final stretch, the body follows common end-of-life changes that can look alarming even when they are expected.

1. Pushing food or water when the body is shutting down
Families often equate feeding with caring, so a loved one’s refusal to eat or drink can feel unbearable. But declining appetite and thirst are widely recognized as a normal part of dying. As swallowing becomes harder, attempts to give food, fluids, or pills can trigger coughing, choking, or visible distress.
Comfort care usually shifts away from intake and toward moisture and mouth care. A damp sponge, lip balm, or ice chips if the person can safely manage them may ease dryness far better than insisting on a full sip or bite. The National Institute on Aging notes that losing one’s appetite is a common and normal part of dying. At the bedside, comfort matters more than completing a meal.

2. Talking about the person instead of to them
Unresponsiveness can make families assume connection is gone. It is common for conversations in the room to shift into planning, medical talk, or emotional discussion as if the dying person is no longer aware. That can be a painful mistake. End-of-life guidance for families and clinicians consistently advises speaking directly to the person, introducing oneself, and keeping words respectful and calm because hearing may remain late into the dying process. Even when eyes stay closed and responses stop, touch and voice can still provide reassurance. A hand on the shoulder, a familiar memory, or a simple “I am here” often fits the moment better than bedside chatter over the person.

3. Mistaking restless or unusual behavior for intentional anger
Terminal restlessness can be one of the hardest signs for families to witness. A person may pull at sheets, fidget, speak oddly, become confused, or seem unlike themselves. These changes can look personal, but they are often linked to the body’s decline, not to unresolved feelings toward the people in the room.

Terminal agitation may happen in the final days and can reflect chemical changes, reduced oxygen, medication effects, pain, fever, constipation, or urinary retention. The most helpful response is usually not arguing, restraining, or demanding clarity. A quieter room, gentle reassurance, reduced stimulation, and help from hospice or palliative staff are the usual supports. Families do not need to decode every word. They need to protect comfort.
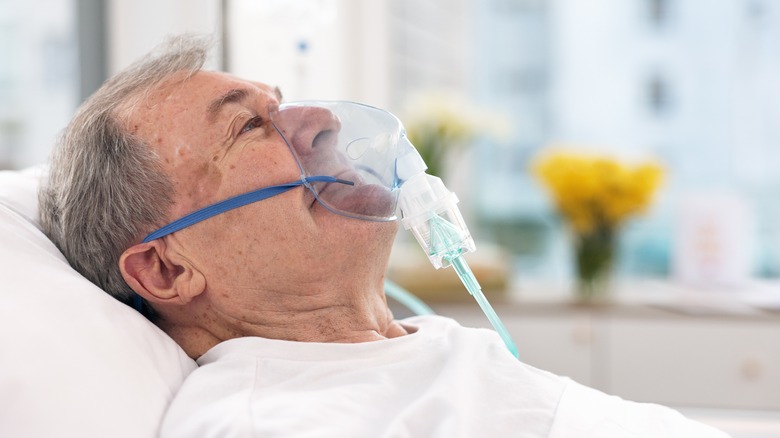
4. Panicking over breathing changes and the “death rattle”
Irregular breathing can frighten everyone in the room. There may be shallow breaths, pauses, bursts of faster breathing, or a rattling sound from secretions collecting in the throat and upper airways. To many families, it sounds like suffering.

Clinical end-of-life education explains that periods of no breathing and rattling congestion are common as death nears. These sounds are distressing to witness, but they do not automatically mean the person is in pain. Raising the head of the bed, turning the person gently, and moistening the mouth are common comfort measures. Panic, repeated shaking, or urgent demands for the person to “breathe” can intensify the room’s distress without helping the patient.

5. Filling the room with conflict, noise, or frantic activity
The bedside can become crowded fast. Relatives arrive, disagreements flare, phones ring, and someone starts trying to manage everything at once. In a family crisis, that can happen almost without notice. Yet the dying person often benefits most from a quieter environment. Dimmer lighting, fewer voices, soft music if desired, and a calm tone can reduce overstimulation. Hospice guidance also advises against arguing with the person, correcting every confused statement, or contradicting comforting visions or perceptions unless they are causing fear. A longer, slower presence usually helps more than hurried motion around the bed. Sitting still, holding a hand, reading a familiar passage, or simply breathing steadily nearby may be the most supportive act in the room.
Life’s final hours rarely unfold in a neat or predictable way. Families do not need perfect words or perfect timing to help. What matters most is recognizing that the body is changing, that many visible signs are expected, and that comfort often comes from gentleness rather than intervention. In the end, a peaceful bedside is usually built from simple acts: moistening dry lips, speaking with respect, lowering the noise, and staying present.

