
The final days of life often bring physical and behavioral changes that can be difficult to witness. While every person’s experience is different, hospice and palliative care sources describe several patterns that commonly appear as the body slows down. Recognizing these signs can help families focus on comfort, communication, and support. These changes do not follow a strict order, and they do not reveal an exact timeline, but they can signal that death is drawing closer.
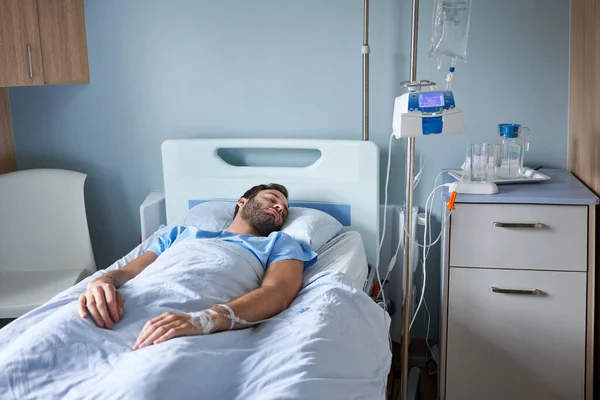
1. Sleeping much more and becoming hard to wake
One of the most common changes is a sharp drop in energy and alertness. A person may spend most of the day asleep, speak less, and become difficult to rouse. As this deep fatigue progresses, they may stop responding to questions or touch in the usual way. Talking and physical activity decrease significantly as death nears. Even when responsiveness fades, hearing may still remain for some time, so calm conversation, a familiar voice, and gentle touch can still be meaningful.

2. Eating and drinking very little
Loss of appetite is a normal part of the dying process. A loved one may take only a few sips of water, decline meals, or stop wanting food altogether. Swallowing can also become harder, which may lead to coughing or choking when food, fluids, or medicine are offered. This change usually reflects the body’s reduced need for fuel rather than a lack of care or will. Comfort measures often shift away from trying to increase intake and toward moistening the mouth, keeping the lips from drying, and giving medications in forms that are easier to tolerate.

3. Breathing that becomes irregular, noisy, or pauses between breaths
Breathing often changes noticeably near the end of life. It may become shallow, rapid, or uneven, with pauses that grow longer over time. Some people develop a pattern of several breaths followed by a stop, then breathing resumes again; this is commonly described as cyclical episodes of apnea and hyperventilation in Cheyne-Stokes respiration. Families may also hear a wet, gurgling sound caused by secretions collecting in the throat. This is widely known as the death rattle. Although it can be upsetting to hear, hospice sources note that it does not usually mean the person is in pain. Repositioning the head or body may reduce the sound and improve comfort.

4. Restlessness, confusion, or sudden agitation
Some people become unsettled in the last days of life. They may pull at bedding or clothing, fidget, toss, or seem unlike themselves. Others appear confused, disoriented, or briefly angry without a clear cause. This is often called terminal agitation or terminal restlessness. It can happen as oxygen levels fall, organs slow down, medications affect brain function, or discomfort builds. In many cases, reassurance, a calm environment, and guidance from hospice or palliative care clinicians are central to keeping the person as comfortable as possible.
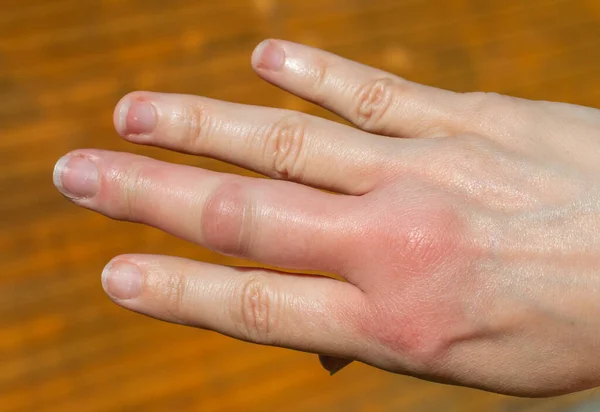
5. Cool, blotchy, or changing skin color
As circulation slows, the skin may feel cooler, especially on the hands, feet, arms, and legs. Color can shift as well. Skin may look pale, gray, purplish, or mottled, particularly over the knees, feet, hands, ears, or buttocks. These changes reflect the body redirecting blood flow away from the extremities. Families sometimes notice that blankets help with comfort, but direct heat sources are generally avoided because fragile skin can burn easily.
6. Less urine and loss of bowel or bladder control
Near the end of life, kidneys may produce less urine, and urine may appear darker than usual. At the same time, bladder and bowel control can weaken. Some people become incontinent, while others may retain urine or become constipated.

This can be a practical and emotional challenge for caregivers, but it is a common sign of physical decline. Care at this stage often centers on skin protection, cleanliness, and reducing discomfort during repositioning or hygiene care.

7. Withdrawal from surroundings or talking about things others do not perceive
A loved one may gradually detach from everyday conversation, favorite activities, or the people around them. Some become quiet and inwardly focused. Others speak about seeing deceased relatives, taking a trip, or preparing to go somewhere. Hospice organizations describe these experiences as part of the sensory and awareness changes that can occur near death. These moments may be comforting, confusing, or emotionally intense for families. A steady presence often matters more than correcting what is said.

Many end-of-life care sources advise speaking gently and assuming the person can still hear, even if they no longer answer. These signs are common, but no single change can predict the exact moment of death. Some appear over days, while others emerge only in the last hours. What remains consistent is the goal of comfort. A quiet room, soft speech, mouth care, repositioning, and support from hospice or palliative care professionals can help families respond to these changes with steadiness and care.

