
Of course, people don’t all describe having the same final moments. But a few patterns keep showing up when medical staff & researchers compare notes, with some being physical, and others being far stranger. These reports have come from hospice teams and bedside observations over the years. Here are nine things people claim to experience right before death.

1. Seeing deceased loved ones
You probably won’t be surprised to learn that a lot of patients claim to see their dead relatives before death. Hospice physician Dr. Christopher Kerr conducted a study of over 1,000 patients and found that many of them said they could see their dead relatives quite vividly. However, they said they felt calm when they saw them, rather than frightened.
The patients also said that they felt more like they were actually encountering these individuals, rather than simply dreaming them. A few of them spoke to them. For other people, it’s more like they’re being visited or guided into the afterlife. The sheer consistency of who appears (almost always familiar people) is something that clinicians have taken note of.

2. Hearing or seeing things others don’t
Similarly, lots of dying people start seeing or hearing things that other people don’t. There are two kinds of hallucinations, those known as delirium-related hallucinations and those known as end-of-life visions. The first kind of hallucinations often involves patients feeling confused or distressed by the things that only they are experiencing.
The second kind of hallucinations tend to be more calm & structured, such as seeing a person or hearing a voice that makes sense in context. These sorts of hallucinations tend to happen without the kind of agitation you might expect from normal hallucinations, and that’s part of the reason that researchers like Dr. Kerr are so interested in them.

3. Feeling like they’re getting ready for a trip
Beyond the behavior, we can’t forget the language that people use when they’re close to death, and many people use vocabulary related to leaving or waiting. Dr. Kerr’s hospice research found that patients often talked about trains or buses, as well as needing to go somewhere. It didn’t matter that they were physically unable to move.
In fact, some would go as far as asking for their shoes and comment on how they were “almost ready” to leave, with Dr. Kerr’s term categorizing these phrases as “journey metaphors.” These appeared among patients across different cultures. Sure, some of the details were slightly different, yet the idea of preparing to go somewhere stayed the same with these patients.
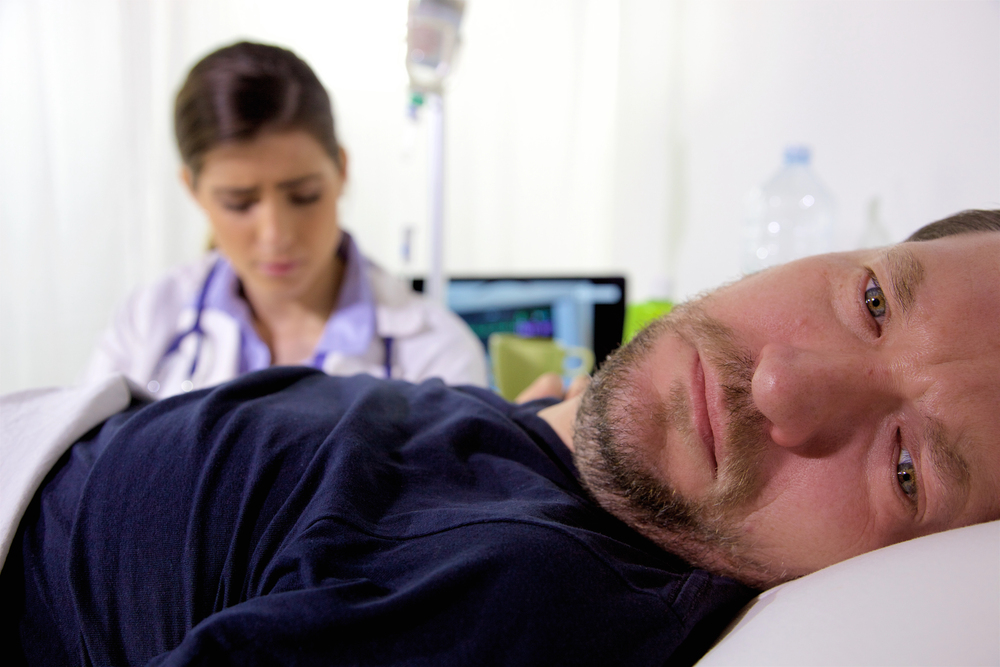
4. Becoming suddenly clear and alert
It’s harder to explain this one because it goes against what you might expect. Apparently, despite being confused or non-responsive for days, lots of patients close to death start speaking clearly. Medical professionals refer to it as “terminal lucidity,” and it’s something that neurologists like Dr. Michael Nahm have documented among dementia patients.
Previously, people may have been unable to recognize family members for months, yet they’re suddenly able to hold full conversations & recall names when they’re close to the end. It might last a few minutes in some people. It might last hours in others. Either way, it appears that terminal lucidity is quite common in people on their deathbeds, although researchers don’t agree on why it happens.

5. Sleeping almost all the time
You’ll see practically every hospice guide talking about patients sleeping a lot towards the end, although it’s more than them simply feeling tired. They’ll drift in & out, and it’s hard to interrupt them when this happens. Many people spend a lot of their time asleep when they’re close to death, and they become a lot harder to wake, which is a sign that their body is slowing down.
Both circulation and brain activity start to drop off at this time. In fact, a lot of families say they feel that the person is fading in & out, sometimes opening their eyes briefly before slipping back into sleep. It’s like they’re unable to fully stay awake, and it can be a little scary to witness for yourself.

6. Losing interest in food and water
No, people don’t simply decide to stop eating during this time. The issue is that it has become physically difficult or unappealing altogether, mostly because the body no longer processes food in the same way anymore. Swallowing becomes a lot harder for them. As a result, it’s common for patients to refuse food they previously loved, and they might even say they’re not hungry at all.
But that doesn’t mean you should start force-feeding them. Far from it. Trying to make someone eat can make them feel uncomfortable, and you don’t really want someone’s last days to be spent that way. Rather than being reduced, a lot of people on their deathbeds stop making meals part of their day entirely.
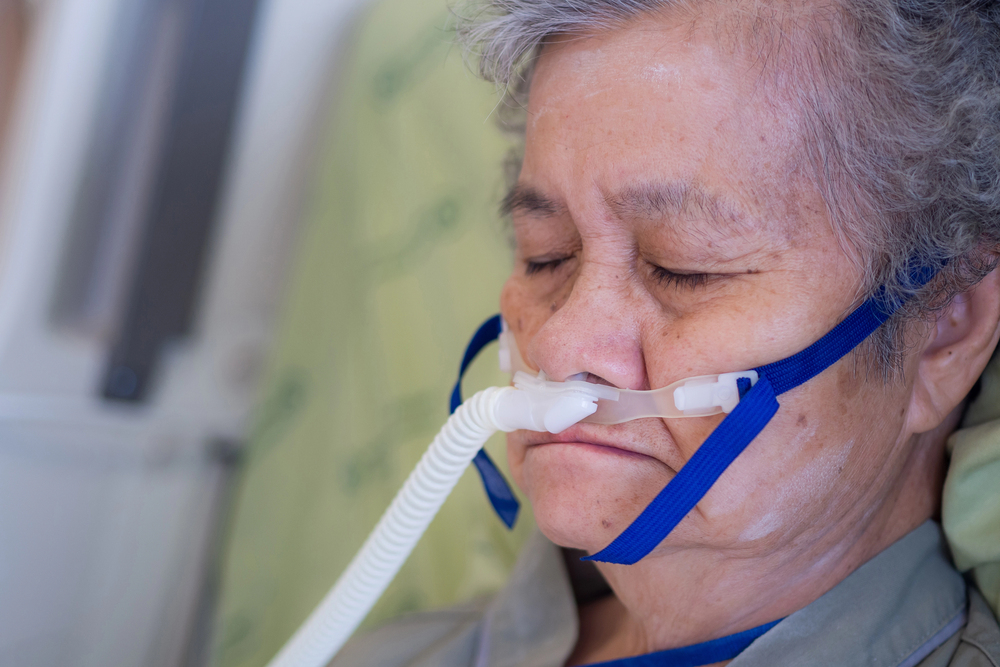
7. Feeling short of breath or unable to get a full breath
It’s quite common for dying individuals to have problems catching their breath, mostly because it feels shallow. The National Cancer Institute explained that dyspnea, or shortness of breath, happens because the body becomes weaker, and there’s sometimes a breathing pattern called Cheyne-Stokes breathing.
This is when someone’s breaths alternate between deep & shallow with pauses in between. Of course, patients don’t always describe the patterns themselves when they’re happening to them, but they will notice the sensation. Breathing no longer feels automatic for them. Instead, it’s something they’re far more conscious of, and likely to be struggling with as well.

8. Becoming restless, agitated, or confused
Unfortunately, not everyone becomes calmer at the end, and there are those who actually experience the opposite. They become uneasy & frustrated, or perhaps confused. Delirium is sadly another common medical condition during the final days, and this can include things like restlessness and agitation. Some people stop recognizing their surroundings.
The cause? According to the National Cancer Institute, it’s changes in the body, like dehydration and shifts in brain chemistry, that cause people’s behavior to change. We also can’t forget the effect of medication on someone’s actions. Even people who used to be quite settled may start moving around and picking at things. They may start speaking in ways that seem normal.

9. Still hearing familiar voices after they stop responding
A 2020 study by Dr. Borjigin & his colleagues focused on brain activity in unresponsive patients when they were close to death. The results were pretty surprising. The researchers found evidence that seemed to suggest a person’s hearing may still work when they’re unresponsive, even though they’re not able to respond themselves.
It’s quite common for patients to be able to process voices late into the dying process, and that’s one of the reasons medical staff encourage families to keep talking. It’s not necessarily due to belief. No, it’s more because there are measurable brain responses in those close to death.
These reports clearly show a mix of responses among dying individuals, including physical changes that you can measure, as well as things people experience. It’s due to these issues that end-of-life care tends to look at more than simply the body. It also focuses on what people say, regardless of how unusual it may seem.

